

Going in for the surgery certainly wasn't the most fun we've ever had. Of course, that is to be expected. The preoperative appointments went quite well.
Dr. Cohen explained to us how the surgery would go and what they would be doing. The surgery was endoscopic, and they would make two incision in Gage's head and remove some bone to help to reshape Gage's head. I've reproduced the quick sketch he gave us below, along with some notes as to what it all means.
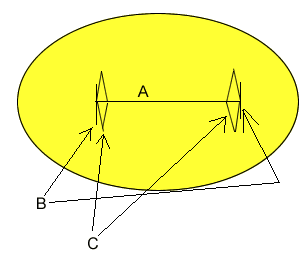
A is the fused suture. They opened this up during the surgery, removing the fused portion of the bone.
B is where they made the two incisions.
C is where they removed more slivers of bone to make the reshaping go more quickly.
The other pre-op appointment was with the people who will be handling the helmet therapy. They took pictures and measurements of Gage's head, something that will continue throughout the helmet therapy, expected to take about 3-1/2 months, more or less, depending on how fast Gage's head shape changes.
The day of the surgery I had to stop feeding Gage about 4 hours before the surgery was scheduled to start. He could have water or Pedialyte up to 3 hours before the surgery. The doctor's office was kind enough to call us about an hour before check in time to let us know things were running behind and that we could give him just a little more water, but we still needed to check in at the same time.
Checking in was pretty easy, and the staff were very good about explaining how things would go. Children's Hospital is a very confusing place, so the surgical registration office gave us written instructions on how to get from their office to our next stop, where Gage was examined. The waiting room was just across from there. Gage had just gotten over a cold mere days before, which was one thing they made note of, but it did not necessitate rescheduling the surgery, thank goodness.
When it was close to the time of the surgery, the anesthesiologist called us in and explained how things would go. The surgery itself would take about two hours, but it could take an additional half hour to an hour for Gage to wake from the anesthesia. When the time for the surgery came, the nurses took Gage from us and sent us to the waiting room.
The time actually went very quickly. Before I expected it, they called for one of us (yes, just one) to come to the recovery room. As the mother and food source, of course I went. The signs weren't as clear as they could be as to where the recovery room was, but I got someone to point it out to me.
Gage was decidedly not interested in eating when he finally woke up. I held him, but he just snuggled in and went back to sleep. Very cozy, but I was quite eager to feed him. He was quite determined to remain asleep, so eventually they moved us to a room.
We ended up in a double, not a single, unfortunately, so our nights were not as quiet as I might have liked. For those of you who have never stayed in a hospital room other than as a patient, let me just tell you, the rumors are true. Those chairs that unfold into beds are really uncomfortable!
Gage continued to refuse to eat, and eventually I went to dinner, leaving Gage with my husband. One wonderful thing the cafeteria at Children's Hospital here in San Diego has is two shiatsu massage chairs, 3 minutes for $1. Great way to cope with the tension.
At 1in the morning, I finally gave in and asked for a breast pump. Naturally, at 1:30, Gage finally wanted to eat. Good thing I hadn't pumped too hard, just took off enough for comfort. Then at 2 the other bed was filled by another infant. It made for a very long night.
Gage did finally start eating regularly later that day. His first feeding in the morning was light, but the feedings after that were more substantial.
He was kept on morphine for the first day after the surgery. They also gave him steroids (I guess he can't play baseball for a while, LOL). The doctors said we could take him home that day if we wanted, but after I explained that we have a 3 year old at home, they understood and let us take an extra night. However, at 8 the next morning, the nurse came in and told us the discharge paperwork was ready to go!
Gage was fortunate and did not need blood, however, his hematocrit and hemoglobin were just a touch low, so he was put on one week of iron therapy. This is not a fun medication to give. I gather it tastes simply horrible. He also has to take a stool softener to ensure that he doesn't get constipated. Finally, we also have Tylenol with codeine to keep the pain under control. I am happy to say we have needed that one very little so far at home.
Next comes the appointments to cast his head for his helmet therapy, then the appointments for that. I can hardly wait to see the finished result. I can already see small differences in the shape of his head and face. The hardest part to deal with right now is that the line down the middle of his skull where they removed the closed suture is very soft, so it's very unnerving touching the top of his head.
Getting the CT Scan
One of the big steps toward the formal diagnosis of craniosynostosis.
Head Casting Pictures
Watching my son get his head cast was so hard yet so fascinating! You never know if your child will be calm about the process or not.
The DOC Band® Helmet
This is what does the shaping of your baby's head after the surgery. Believe it or not, my son missed it once it was gone.
Scaphocephaly Pictures
Pictures of my son before and during treatment for scaphocephaly/craniosynostosis.
Copyright © 2003-2026 Stephanie Foster unless otherwise indicated
![]()
![]()
![]()
![]()
![]()
![]()
![]()
Home With the Kids on LinkedIn
Ads
Free Mini-Course
Find out if becoming a general transcriptionist is the right career choice for you. This all-inclusive online education system will teach you general transcription.
Career Step
Want to be a medical coder or transcriptionist? Career Step provides quality training for people wanting to enter these fields and more..
Ads
25+ Basic Life Skills Parents Need To Teach Their Kids
Disclosure: Home with the Kids is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to amazon.com. I also review or mention products for which I may receive compensation from other sources. All opinions are my own.